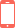
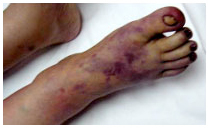
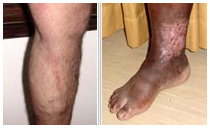
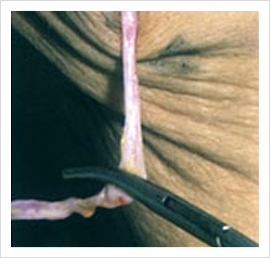
Varicose Vein Stripping
LSV surgery
This operation is nowadays done rarely and has been replaced with Endovenous abalation.
- Trendelenberg position with 20 - 30° head down
- Legs abducted 10 -15°
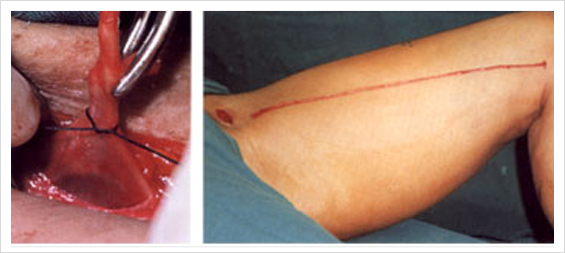
- Saphenofemoral junction (SFJ) found 2 cm below and lateral to pubic tubercle
- Essential to identify SFJ before performing flush ligation of the LSV
- Individually divide and ligate all tributaries of the LSV
- Superficial circumflex iliac vein
- Superficial inferior epigastric vein
- Superficial and deep external pudendal vein
- Check that femoral vein clear of direct branches for 1 cm above and below SFJ
- Stripping of LSV reduces risk of recurrence
- Only strip to upper calf.
- Stripping to ankle is associated with increased risk of saphenous neuralgia
- Post operative care:
- Elevate foot of bed for 12 hours
- Class 2 stockings should be worn for at least 2 weeks
SSV surgery
- Patient prone with 20-30° head down
- Saphenopopliteal junction (SPJ) has very variable position
- Preoperative localisation with duplex ultrasound is strongly recommended
- Identify and preserve the sural nerve
- Need to identify the SPJ
- Stripping associated with risk of sural nerve damage
- Subfascial ligation inadequate
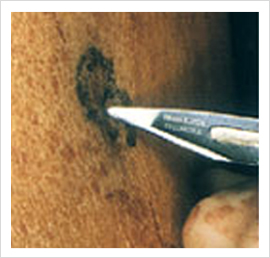
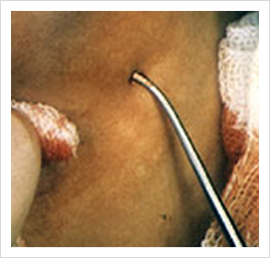
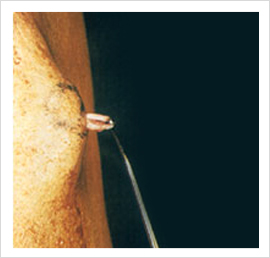
Ambulatory Phlebectomy (Multiple Stab Avulsion)
Large veins are best treated with this method as it does not lead to thrombophlebitis and skin pigmentations. This procedure is always combined with abalation of LSV or SSV. The veins are marked pre-operatively. Stab incisions are made along the blow outs. With Phlebectomy hooks, the veins are avulsed at multiple points. Wounds are closed with steri strips.
This surgery is performed as a day care operation where the patient can go home the same evening and has no stitches in his legs.
Perforator surgery
- Significance of perforator disease is unclear
- Perforator disease may be improved by superficial vein surgery
- Perforator surgery (e.g. Cockett's and Todd's procedure) associated with high morbidity
- Subfascial endoscopic perforator surgery (SEPS)
- Not indicated for uncomplicated primary varicose veins
- May have a role in addition to saphenous surgery in those with venous ulceration
Dr. Pankaj Patel a vascular surgeon has expertise in peripheral vascular diseases, varicose veins and deep vein thrombosis
TO FIND A VARICOSE VEINS OR SPIDER VEINS CENTER NEAR YOU, VISIT veinsonline.com