Raynaud's disease is a condition that affects the blood supply to the fingers, toes and occasionally the ears and nose. During a Raynaud's attack, the blood vessels constrict (narrow) and blood supply to these area reduces. This results in colour changes in the skin, often accompanied by a throbbing or burning sensation, cold, and numbness. The exact cause of Raynaud's disease remains unknown. Research is going on to establish its exact cause.
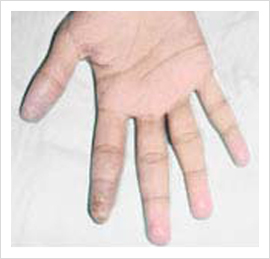
During a typical Raynaud's attack the affected area may first become white (pallor) as the blood supply is reduced, then blue (cyanosis) as the oxygen supply to the area is depleted, followed by bright redness (rubor) as the blood returns to the area (reactive hyperemia). Raynaud's disease, by definition, involves three color changes. However, neither do they occur in every patient nor is the order of colour change consistent.
Raynaud's episodes can be triggered by cold, either by touching cold objects or by being in a cold environment. Emotions such as stress and anxiety may also play a role. The severity of attacks will vary from episode to episode, as well as from patient to patient. Attacks typically last a few minutes.
Raynaud's disease occurs more frequently in women than in men. Although it can occur at any age it usually begins between the ages of 15 and 40. It is estimated that 4 - 5% of the population is affected.
Raynaud's is divided into two categories
Primary Raynaud's or Raynaud's disease, occurs when an individual has only the above mentioned colour changes along with the typical symptoms of pain or numbness. There is no other medical problem which could be causing these episodes.
Secondary Raynaud's or Raynaud's phenomenon, occurs when the Raynaud's episodes are secondary to or associated with another medical condition causing these attacks. Or, Raynaud's is only one of the symptoms associated with the other disease. Although this form is less common than primary Raynaud's, it is a more complex and serious disorder. Some examples of other underlying diseases associated with Raynaud's are: connective tissue diseases, scleroderma, rheumatoid arthritis, lupus, vibration white finger, occlusive arterial disease, thoracic outlet syndrome, carpel tunnel syndrome.
Primary Raynaud's disease is diagnosed following criteria described by Allen Brown criteria
Additional tests might help in making the diagnosis
There is no known cure for this condition, therefore, various supportive treatments are essential. Most cases of primary Raynaud's can be controlled with proper medical care.
What you can do
Many people are able to find relief by simply adjusting their lifestyle. For example
What a doctor might do
For more severe cases that require medication, your doctor might prescribe drugs which keep your blood vessels from narrowing and help them dilate (expand), such as Nifedipine, Diltiazem, or Nitroglycerin. Some of these medications may have side effects which you should discuss with your physician before taking.
Non-medication treatment
Biofeedback has been demonstrated to be a safe and effective remedy for some individuals. This is a technique designed to help a person gain control over involuntary body functions, such as skin temperature, heart rate, or blood pressure. Biofeedback training is necessary and several methods are available.
Surgery
In rare instances, a sympathectomy may be performed. This operation cuts the nerves that may also be affecting the blood vessels to the fingers. This procedure may not be that effective and may work only for a short period of time.
Surgical and Other Invasive Treatment
If medical measures are not sufficient, surgery or balloon angioplasty may be advised. There are 2 major types of operations: Surgical revascularization, in which the blocked arteries are bypassed with either healthy blood vessels taken from elsewhere in the body (usually a vein in the leg) or use of a synthetic graft; and endartectomy, which involves opening portions of the diseased artery and removing the atherosclerotic deposits.
Balloon angioplasty, in which a catheter with a balloon tip is inserted into an artery and inflated to compress the fatty deposits, is most successful for people with small segments of blockage. However, the area becomes quickly reclogged in about 30 percent of all cases, requiring repeat treatment within a year or two.
Dr. Pankaj Patel a vascular surgeon has expertise in peripheral vascular diseases, varicose veins and deep vein thrombosis